Introduction
Atherosclerosis, a chronic disease of the arteries that manifests itself with thickening and hardening of the vascular wall, is a primary cause of serious cardiovascular events such as stroke, heart attack and peripheral vessel occlusion.
The prevention of atherosclerosis can be significantly influenced by the management of cholesterol levels, particularly through the adoption of a diet rich in nutraceuticals with vascular anti-inflammatory properties. LDL cholesterol, often described as “bad” cholesterol, tends to build up on the walls of blood vessels, forming plaques that narrow and harden the arteries. This dietary approach, aimed at keeping cholesterol levels low and preventing the adhesion of cholesterol to arterial walls, represents a key strategy in the prevention of atherosclerosis and related cardiovascular complications.
In this context, substances such as gamma-oryzanol present themselves as potential therapeutic agents in the control of vascular inflammation linked to atherosclerosis.
Inflammation plays a crucial role in atherosclerosis, characterized by a persistent, low-grade inflammatory state in the arteries. Immune cells such as macrophages, lymphocytes and mast cells are actively involved in the formation of atherosclerotic plaques, creating a vicious cycle with fat accumulation and inflammation [1].
The initial stages of atherosclerosis see both the deposition and chemical modification of fats, which through oxidation processes activate immune cells and promote the release of pro-inflammatory mediators [2]. This chronic inflammation is an alteration of the balance between pro- and anti-inflammatory mediators, leading to ineffective resolution of the inflammatory process [3].
An important aspect in atherosclerosis is endothelial cell dysfunction. These, in response to physical or chemical stress, undergo an alteration of their functional phenotype, expressing inflammatory molecules and favoring the recruitment of immune cells [4].
Cell adhesion molecules, such as ICAM-1 and VCAM-1, play a significant role in modulating inflammatory interactions and could represent interesting therapeutic targets [5].
Anti-inflammatory strategies have shown effectiveness in reducing cardiovascular events and mortality, underscoring the need to manage risk factors and develop new therapeutic approaches [6,7]. The importance of inflammation in atherosclerosis is further strengthened by successes in treating the disease through modulation of immune responses, both innate and adaptive [8].
Immunomodulation, as well as the adoption of a careful diet and targeted food supplementation, are among the most promising approaches in this area [9].
In this panorama, gamma-oryzanol emerges as a promising substance for its anti-atherosclerotic potential, acting on the mechanisms of vascular inflammation, and represents an important topic of investigation for the treatment and prevention of cardiovascular diseases.
Experimental part
In vitro pro-atherogenic anti-inflammatory activity tests were performed on endothelial cells of the HUVEC line (ATCC), activated in an inflammatory sense by stimulation with IL1-B or with TNF-A and treated with increasing concentrations of Gamma-Oryzanol “Oryzox” (ie 31.25, 62.5, 125 ?g/ml). To estimate the effect of GAMMA-ORY on the regulation of inflammation, the membrane expression of ICAM-1 and VCAM-1 proteins was quantified by flow cytometry (FACS), respectively by labeling with anti-ICAM- antibodies 1 Alexa-633 and anti-VCAM-1 Alexa-488. The solubility of the sample under analysis was evaluated in different solvents and once the best condition had been ascertained, cellular toxicity tests were carried out at the times of 24, 48 and 72h and at the above concentrations.
None of the conditions analyzed resulted in cytotoxicity of either the preparation in solution or the vehicle used. We therefore opted for the 72h timing as the one to treat cell cultures with GAMMA-ORY. Given that the results of the preparatory FACS tests, the experiment showed a lower expression of ICAM-1 and VCAM-1 with the induction of IL1-B compared to that with TNF-A (both stimuli 24h), it was preferred to use the latter at a concentration of 10ng/ml for the stimulation of the in vitro inflammatory model (Fig.1). The final results of the experiment are shown in Fig.2 which shows the data on the effect of the treatment with GAMMA-ORY in terms of percentage compared to the positive control (i.e. cells only activated with TNF-A, 100% activation).
Expression of adhesion molecules in flow cytometry
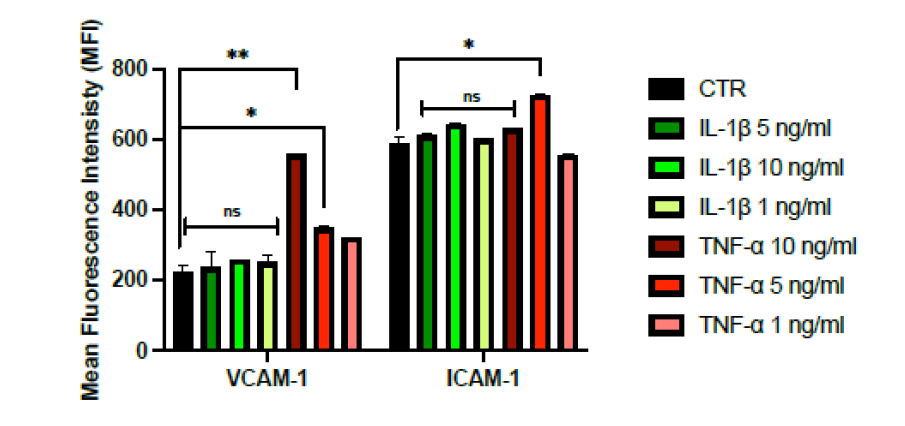
Fig.1. Outcome of stimulation with IL1-B and TNF-A on the expression of VCAM-1 and ICAM-1 . HUVEC cells were activated with the two pro-inflammatory stimuli at the concentrations indicated in the legend for 24h (CTR, untreated). Do the expression values reach statistical significance essentially following stimulation with TNF-A at concentrations of 5 and 10 ng/ml..
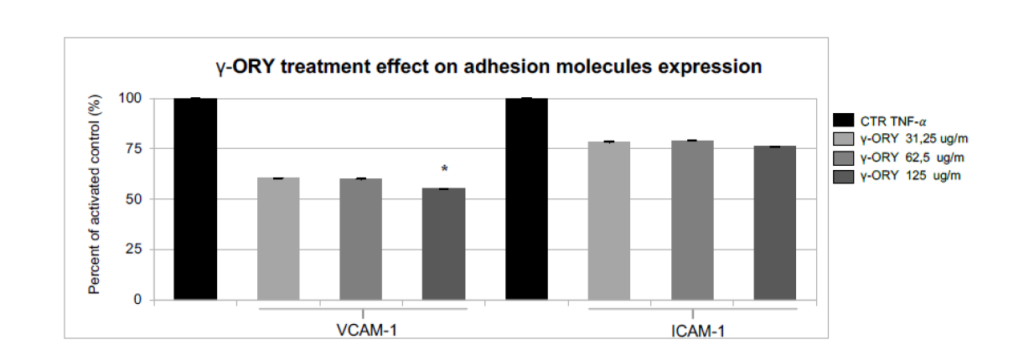
Fig.2. Effect of Gamma-Oryzanol treatment on VCAM-1 and ICAM-1 expression. Cells activated with TNF-A (10 ng/ml, 24h)
were incubated for 72h with GAMMA-ORY (doses in legend) or not (CTR TNF-A). The estimate of the treatment effect is reported as the
percentage of VCAM-1 and ICAM-1 expressed in the GAMMA-ORY-treated condition compared to the untreated condition (100%, TNF-A Control activated). (*) Statistical significance of VCAM-1 expression treated with GAMMA-ORY 125 ug/ml vs CTR not treated with the substance (p=0.05).
Results
Multiple analyzes were performed to identify appreciable and reliable levels of adhesion markers, such that they were optimally representative of endothelial inflammation. From the experimental set aimed at the quantification of the membrane molecules VCAM-1 and ICAM-1, it appears that the treatment with GAMMA-ORY is effective in modulating their expression and in particular in reducing their levels, consequently decreasing the degree of cellular activation in pro-atherogenic sense. In particular, the expression of VCAM-1 treated with GAMMA-ORY at a dose of 125 g/ml showed a statistically significant decrease compared to the control not treated with the substance (Fig.2.). The values shown in Table 1 indicate how much the expression of each of the adhesion molecules is inhibited in percentage following treatment with increasing doses of GAMMA-ORY compared to no treatment. The absence of treatment is the condition represented by the positive control, consisting of cells activated only with TNF-A and not treated with GAMMA-ORY (i.e. CTR TNF-A, i.e. 100% expression of VCAM-1 and ICAM-1, i.e. 100% pro-atherogenic inflammatory activation).
| Dose di γ-ORY | VCAM-1 | ICAM-1 |
|---|---|---|
| 31,25 μg/ml | 39% | 22% |
| 62,5 μg/ml | 40% | 21% |
| 125 μg/ml | 45% | 24% |
Tab.1. Effect of Gamma-Oryzanol treatment on VCAM-1 and ICAM-1 expression. Values of the percentage reduction in the expression of the two proteins due to the effect of the applied dose, compared to untreated inflammation.
Bibliography
- Libby P, Buring JE, Badimon L, Hansson GK, Deanfield J, Bittencourt MS, Tokgözo?lu L, Lewis EF. “Atherosclerosis.” Nat Rev Dis Primers. 2019 Aug 16;5(1):56.
- Gisterå A, Hansson GK. “The immunology of atherosclerosis.” Nat Rev Nephrol. 2017 Jun;13(6):368-380.
- Zhu Y, Xian X, Wang Z, Bi Y, Chen Q, Han X, Tang D, Chen R. “Research Progress on the Relationship between Atherosclerosis and Inflammation.” Biomolecules. 2018 Aug 23;8(3):80.
- Gimbrone Jr MA, García-Cardeña G. “Endothelial Cell Dysfunction and the Pathobiology of Atherosclerosis.” Circ Res. 2016 Feb 19;118(4):620-36.
- Price DT, Loscalzo J. “Cellular adhesion molecules and atherogenesis.” Am J Med. 1999 Jul;107(1):85-97.
- Bugger H, Zirlik A. “Anti-inflammatory Strategies in Atherosclerosis.” Hamostaseologie. 2021 Dec;41(6):433-442.
- Chistiakov DA, Melnichenko AA, Grechko AV, Myasoedova VA, Orekhov AN. Potential of anti-inflammatory agents for treatment of atherosclerosis. Exp Mol Pathol. 2018. Apr;104(2):114-124.
- Deroissart J, Porsch F, Koller T, Binder CJ. “Anti-inflammatory and Immunomodulatory Therapies in Atherosclerosis.” Handb Exp Pharmacol. 2022:270:359-404.
- Yamashita T, Sasaki N, Kasahara K, Hirata K-I. “Anti-inflammatory and immune-modulatory therapies for preventing atherosclerotic cardiovascular disease.” J Cardiol. 2015 Jul;66(1):1-8.
- Centro di Medicina Biologica srl https://www.centrodimedicinabiologica.it/aterosclerosi-e-infiammazione-vascolare/
